When it comes to our medicines system, it is hard to overstate how profoundly broken it is.
Here in the U.S., many of our neighbors, especially seniors, are forced to choose between paying for medicine or food. Hundreds of cancer physicians recently wrote an angry public letter protesting the fact that one in five of their patients can't afford to fill their prescriptions—not surprising, with the cost of cancer medicines now averaging over $100,000.
Price-gouging anger about drugs like the EpiPen, plus a promising California ballot initiative, and now a strong UN report on access to medicines. Will it all lead to reform of our broken medicines system?
The Altiero Spinelli building of the European Parliament in downtown Brussels exudes modernity. Its steel-and-glass structure houses high-ceilinged hearing rooms with perfect lighting, blonde wood, and state-of-the-art audio and video technology. These spaces seem to embody technocratic competence and calm deliberation, but on a chilly afternoon last December, one of these hearing rooms was the setting for a scathing denunciation of the global system for developing and distributing medicine.
When is a decision on a patent application not a decision at all? When it runs counter to the powerful commercial and diplomatic forces that protect massively profitable pharmaceutical monopolies. Or at least that is what many advocates for access to medicines are saying is the reason behind Indian patent officials last month reversing their own 2015 decision that denied United States-based Gilead Sciences a patent on its hepatitis C treatment sofosbuvir, commonly marketed as Sovaldi. The new decision holds that Sovaldi meets the Indian patenting requirements of novelty and inventiveness. But the earlier decision by the same agency came to the opposite conclusion, holding that Gilead’s drug was not a significant improvement over an already available compound.
Enormous public frustration with the skyrocketing prices of essential medicines in the US has not yet led to any meaningful reform. But a historic initiative on the November ballot in California, championed by health care and consumer advocates and fiercely opposed by multinational drug corporations, may finally rein in Big Pharma.
In response to a letter from access to medicines activists and organizations, the U.S. State Department explicitly acknowledged the TRIPS Agreement right to issue compulsory licenses for pharmaceuticals. The letter can be found below.
Don Reichmuth survived prostate cancer once before, back in 2007, so his physician was concerned when tests recently revealed the cancer had returned. Reichmuth's physician prescribed a drug called enzalutamide, marketed by the Japanese company Astellas Pharma, Inc. under the brand name Xtandi. But when the physician sent the prescription to the pharmacy, the managers of Reichmuth's insurance plan sent back an immediate refusal to approve it.
Reichmuth, a retired teacher who lives in Washington State, was puzzled by the logic. Then he learned the price of the Xtandi prescription: over $9,700 each month.
It is Hannah Lyon’s first-ever experience with public speaking, but she clears her throat, clutches her notes, and plunges in. “Hello. My name is Hannah, and while I might not look like it, I am a cancer patient.”
Lyon’s audience was gathered in front of her on a Washington, DC sidewalk to commemorate World Cancer Day. She explains to them that she was just 26 years old when she was diagnosed with advanced cervical cancer. Her first set of doctors saw Lyon’s best-case scenario as chemotherapy and radiation that would only extend her life for a few years. Desperate for a more promising approach, Lyon found a clinical trial at the National Institutes of Health (NIH). There, she received cutting-edge immunotherapy, where her immune cells were genetically modified and reinserted into her bloodstream. Since the treatment, Lyon’s tumors have shrunk more than 80%.
For most of human history, life-saving drugs were a public good. Now they’re only good for shareholders.
Along the path toward the creation of a global capitalist system, some of the most significant steps were taken by the English enclosure movement.
Between the 15th and 19th centuries, the rich and the powerful fenced off commonly held land and transformed it into private property. Land switched from a source of subsistence to a source of profit, and small farmers were relegated to wage laborers. In Das Kapital, Marx described the process by coining the term land-grabbing. To British historian E.P. Thompson, it was “a plain enough case of class robbery.”
Full disclosure: initially, I was not very excited about the announcement of the convening of the United Nations Secretary-General’s High-Level Panel on Access to Medicines. Every human rights advocate has learned to approach with restraint the news of yet another august group convening to review a crisis.
Such groups can be counted on to issue a wonderful report with promising language. But, almost inevitably, the gauzy, aspirational recommendations in that report are promptly ignored. Worse, in the case of access to medicines, noble but unenforceable calls for reform are reliably bulldozed over by binding trade agreements that elevate corporate profits over human rights.
The flaws of the modern medicine patent system are widely decried. The current system fails to develop medicines to address the health needs of the global poor and creates a platform for unaffordable pricing of the medicines that exist. But even the harshest critics of the patent paradigm recognize the need to provide incentives for vigorous research and development of new medicines. Many alternatives have been proposed. Some are already in operation at limited levels. But these alternatives are poorly understood, even in the global health community.
Mary-Jane Matsolo, wearing tight jeans, gold high-heeled sandals, and a white t-shirt with navy blue block letters reading “HIV Positive,” strides to the front of the Johannesburg conference room. “I’m the one who will make you understand patent laws and intellectual property rights,” she says to the dozen people gathered before her. “It’s what I do, and I do it very well.”
Earlier this month, representatives of the Trans-Pacific Partnership Agreement (TPPA) parties announced they had concluded five years of negotiations by agreeing to final terms. The governments have not yet allowed the public to view the agreement, but a version of the TPPA’s intellectual property chapter published by Wikileaks reveals what I consider a potentially devastating setback to the human right to health.
Pope Francis has warned us about a system that elevates profits above people. "Today we also have to say 'thou shalt not' to an economy of exclusion and inequality," he wrote in his 2013 apostolic exhortation Evangelii Gaudium. "Such an economy kills." In the case of access to medicines, Francis' dire prediction is proven true thousands of times each day.
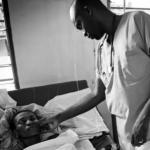
It is hard to imagine an injustice more intolerable than a sick person being blocked from receiving the medicine that would alleviate her suffering, or even save her life. As Archbishop Silvano Tomasi, permanent observer of the Holy See to the United Nations has pointed out, the scope of this tragedy is breathtaking: Two billion people lack access to essential medicines, costing 10 million lives each year.
Part of my job is to work alongside my law students as we represent low-income persons in our Indianapolis-based clinic. Our community does not have a strong public transit system, and many of the available jobs are located far away from where our clients live. Our clients need cars, but they do not have much cash or strong credit ratings. So they turn to the car dealers that populate their neighborhoods, filling concrete lots with shiny vehicles and bright signs promising great cars and forgiving financial terms.
No one understands the value of medicines better than famed Indiana University School of Medicine professor and oncologist Dr. Lawrence Einhorn.
In the mid-1970s, testicular cancer that had spread beyond the abdomen was considered a terminal diagnosis. Then, Dr. Einhorn developed a revolutionary multi-drug approach that transformed the disease into a cancer with a higher cure rate than any other.
Intellectual property protections for medicines are often overlooked in public discussions of U.S. trade agreements. But they shouldn’t be. Negotiations over such intellectual property can mean the difference between antiretroviral medicine that costs over $10,000 per year—the price originally set in the 1990s by monopoly patent holders—and the eventual grudging concessions that dropped the drug prices to less than a dollar a day. For millions of HIV-positive people in the developing world, that price gap is a matter of life and death. The same dynamic applies to patients in need of medicines to treat cancer, heart disease, and any number of other health conditions.
Representatives of Pacific Rim nations are negotiating a trade agreement that could negatively impact the health of millions. But the high-profile discussion about the proposed Trans-Pacific Partnership Agreement (TPPA) also presents an opportunity for health advocates. This Perspective essay first reviews key proposed terms of the TPPA that would extend the flawed pharmaceutical patent regime and violate multiple human rights commitments. Second, the social movement to ensure access to antiretroviral medicines is presented as an object lesson in successful advocacy for health as a human right. Finally, this essay argues that the attention paid to the TPPA by media, lawmakers, and social justice activists, particularly in the US, creates an ideal platform for advocacy in support of the human right to essential medicines.